You board a long-haul flight, settle into your seat, and sit still for hours in a cramped cabin at altitude. What most travellers do not realise is that this scenario is a near-perfect recipe for a deep vein thrombosis (DVT) — a blood clot forming in the leg veins. Dr. Mohamed Haggag, vascular surgeon in Heliopolis, Cairo, explains exactly why the risk arises and how to prevent it on every flight.
Why Does Air Travel Increase DVT Risk?
The explanation lies in what haematologists call Virchow's Triad — three factors that combine to promote clot formation:
- Venous stasis: Prolonged sitting keeps leg muscles inactive, slowing blood flow through the deep veins of the calf and thigh.
- Hypercoagulability: Cabin dehydration from low cabin humidity and alcohol consumption thickens the blood, raising clotting tendency.
- Endothelial injury: Cramped seating can press the back of the knee or thigh against the seat edge, mildly injuring vein walls.
Add reduced cabin pressure and mild hypoxia (lower oxygen), and you have conditions that meaningfully raise DVT risk.
Who Is Most at Risk?
While anyone on a long flight can develop DVT, certain groups face substantially higher risk:
- People with a previous DVT or pulmonary embolism
- Pregnant women and those in the first 6 weeks postpartum
- Passengers with active cancer or recent surgery
- Obese individuals (BMI > 30)
- Those taking combined oral contraceptives or hormone therapy
- Older passengers and those with hereditary clotting disorders (thrombophilia)
How to Protect Yourself: Practical Prevention
The good news is that simple measures dramatically reduce travel-related DVT risk:
- Move every 1–2 hours: Walk the aisle for 2–3 minutes. Even standing and shifting weight helps.
- Calf exercises in your seat: Repeatedly lift your heels and drop them (calf raises), circle your ankles, and flex and extend your toes. Do 10 repetitions every 30 minutes.
- Stay hydrated: Drink water regularly. Avoid excess alcohol and caffeine, which dehydrate.
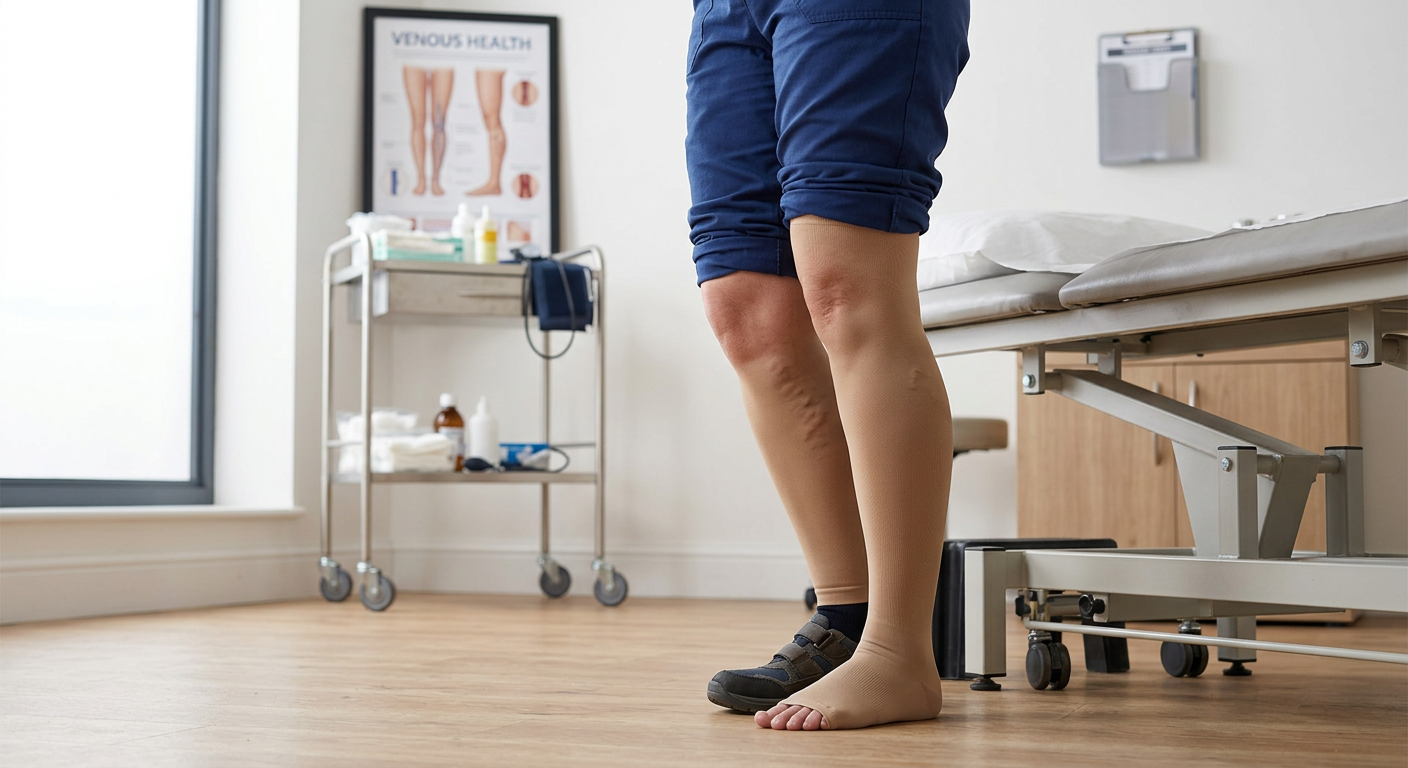
- Wear compression stockings: Class 1 graduated compression stockings (15–20 mmHg) reduce the risk of DVT in long-haul flights by up to 90% in high-risk passengers.
- Aisle seat: Choose an aisle seat so you can stand up easily without disturbing fellow passengers.
- Avoid crossing your legs: This impairs venous return and worsens stasis.
When Should You See a Vascular Surgeon Before Flying?
Book a pre-travel consultation with Dr. Haggag if you:
- Have had a previous DVT or PE
- Are flying within 4 weeks of major surgery
- Have a known clotting disorder (thrombophilia)
- Are pregnant, especially in the third trimester
- Have active cancer
In these cases, preventive anticoagulation (blood-thinning medication taken before and during the flight) may be recommended. This decision must always be made by a physician — do not self-medicate.
Warning Signs After a Flight
DVT symptoms can appear during or up to 2 weeks after a long flight. Seek medical attention promptly if you notice:
- Swelling, pain, or tenderness in one calf or thigh
- Skin redness or warmth over a vein
- A visible cord-like vein
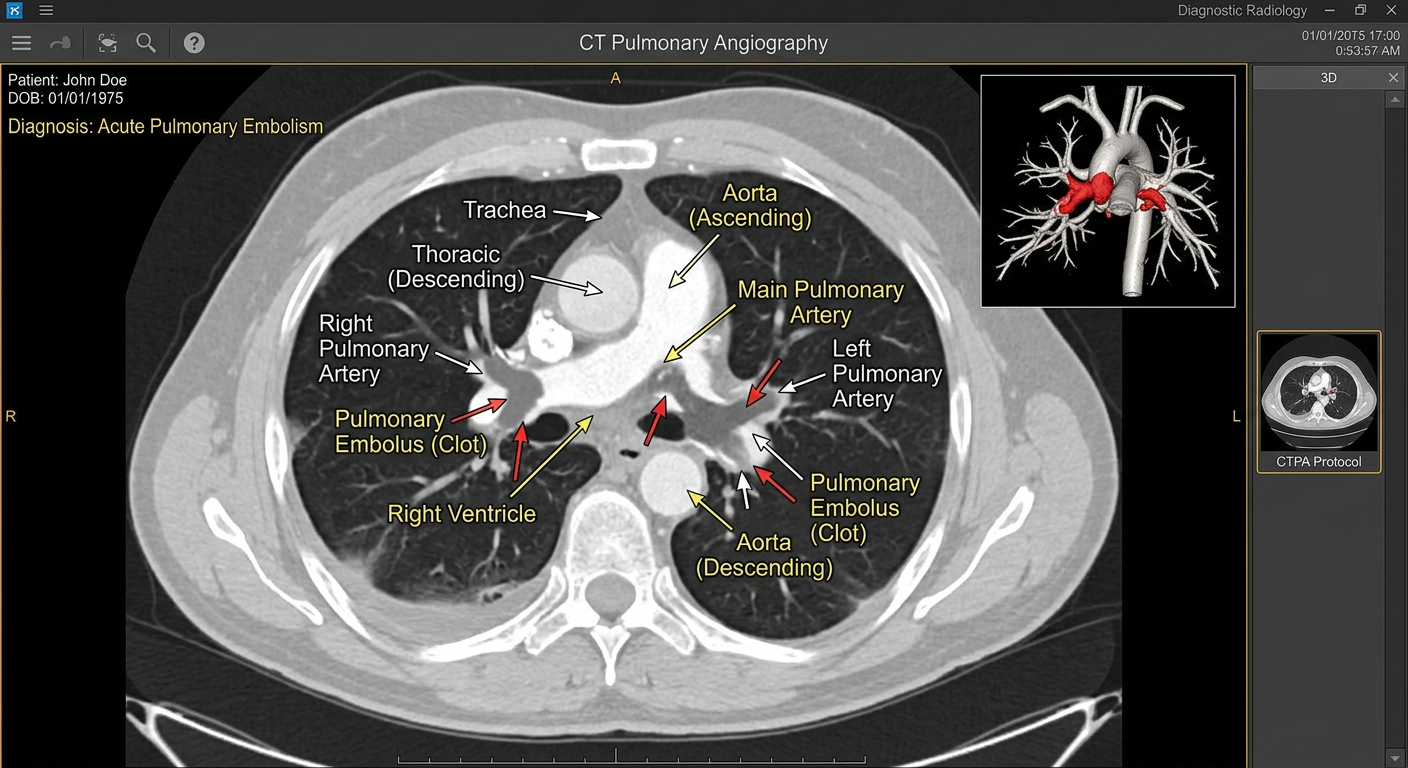
- Sudden shortness of breath or chest pain — these may signal a pulmonary embolism (PE), a medical emergency
Diagnosis and Treatment
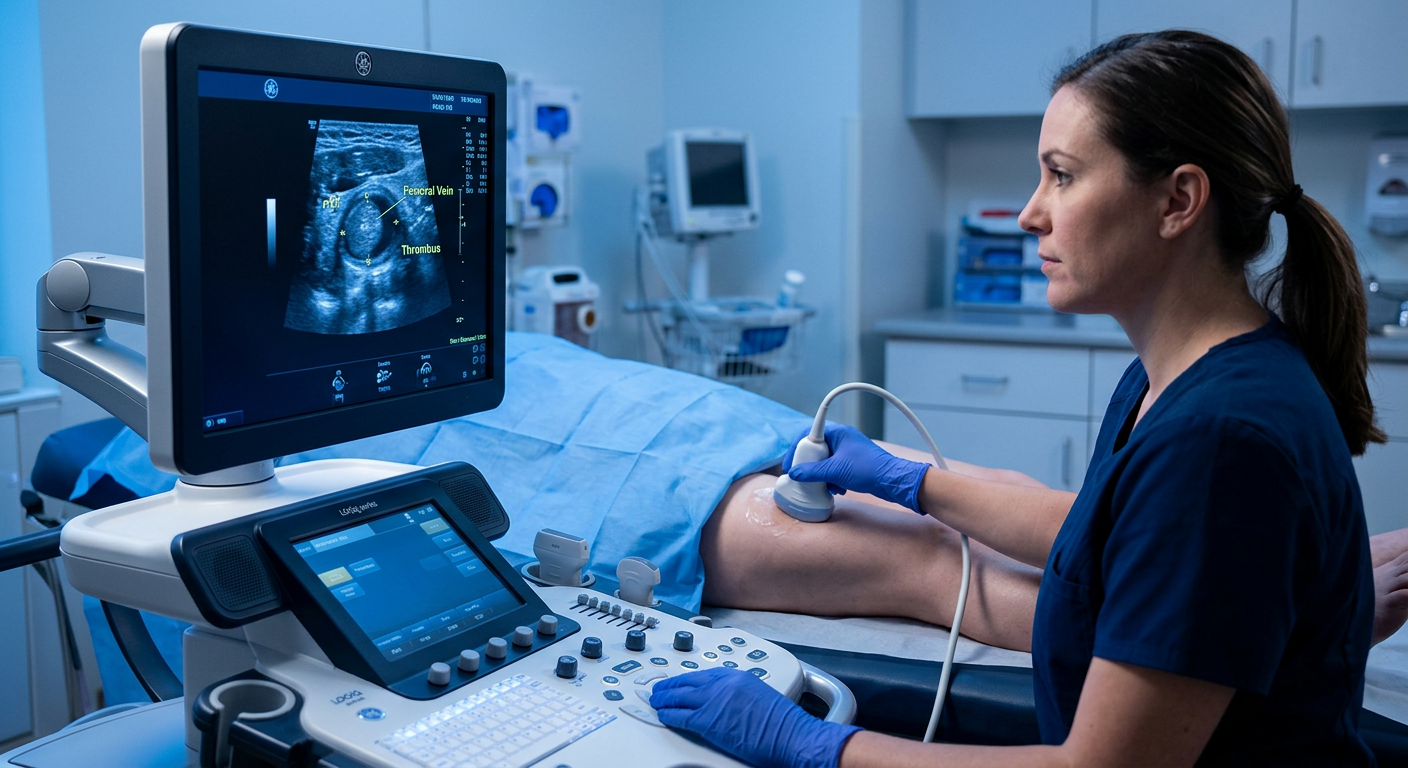
If DVT is suspected, a venous duplex ultrasound confirms the diagnosis within minutes, non-invasively. Treatment depends on clot location and severity but typically includes anticoagulation for 3–6 months and graduated compression therapy. Extensive clots in high-risk patients may be treated with catheter-directed thrombolysis to prevent post-thrombotic syndrome.
Flying Soon? Get a Pre-Travel Assessment
If you have vascular risk factors and are planning a long-haul flight, a short consultation with Dr. Mohamed Haggag can ensure you travel safely.
Book a Consultation