A young woman develops significant swelling in her left leg. Standard blood tests and genetic thrombophilia screens come back normal. A routine duplex ultrasound finds a DVT, but there is no obvious trigger. This scenario — left leg DVT in a young woman with no identifiable cause — is one of the most common presentations of May-Thurner syndrome. The condition is underdiagnosed, treatable, and, when missed, leads to recurrent clots and debilitating chronic venous insufficiency. Dr. Mohamed Haggag, vascular surgeon in Heliopolis, Cairo, explains what May-Thurner syndrome is and how it is treated.
What Is May-Thurner Syndrome?
May-Thurner syndrome (MTS) — also called iliac vein compression syndrome or Cockett's syndrome — is an anatomical variant in which the right common iliac artery crosses over and compresses the left common iliac vein against the fifth lumbar vertebra. This extrinsic compression narrows the vein, impairs venous outflow from the left leg, and creates a predisposition to thrombosis.
The condition was first described by May and Thurner in 1957, who found that 22% of cadavers showed significant compression at this anatomical crossing point. A degree of anatomical compression is present in the majority of the population — it only becomes symptomatic in a subset when physiological stressors (oral contraceptives, pregnancy, dehydration, immobility) are added.
Why Does It Predominantly Affect Women?
May-Thurner is diagnosed far more often in women of reproductive age for several reasons:
- Combined oral contraceptives raise oestrogen levels, which promote clotting and reduce fibrinolysis — the perfect added risk on top of anatomical compression
- Pregnancy increases pelvic blood volume, right iliac artery pressure, and venous stasis — amplifying compression
- Women's pelvic anatomy may result in a slightly narrower angle at the crossing point
- Hormonal influences on vein wall compliance and coagulation baseline differ from men
This does not mean men are immune — MTS does occur in men, but it is considerably less common and is often discovered incidentally during investigation for unilateral left leg swelling or DVT.
Symptoms
Symptoms range from subtle to severe:
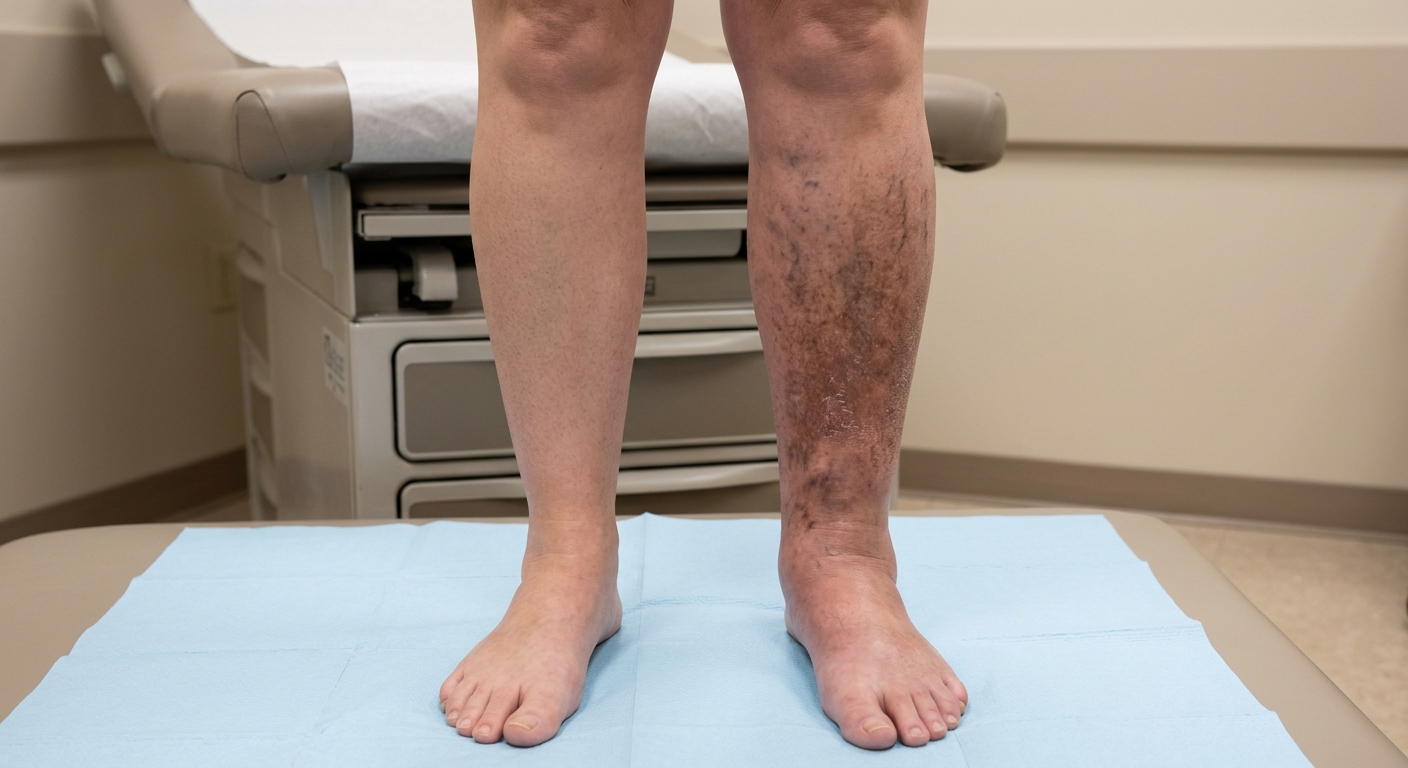
- Left leg swelling — typically the first and most prominent symptom, often worse at the end of the day or after prolonged standing
- Left leg pain or heaviness — a chronic aching discomfort with no obvious cause
- Left-sided DVT — particularly iliofemoral DVT involving the iliac and femoral veins, which carries a higher risk of post-thrombotic syndrome than isolated calf DVT
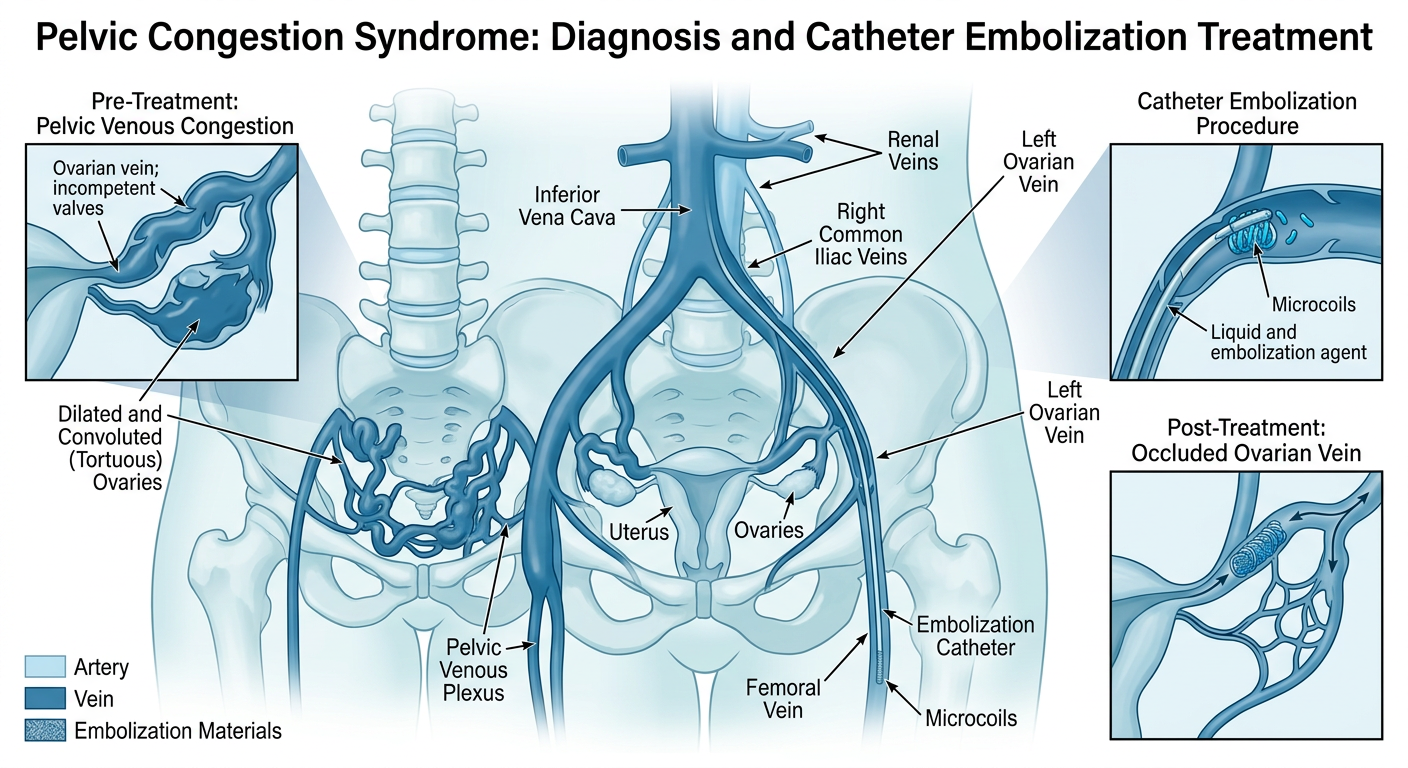
- Pelvic congestion — dilated pelvic veins and pelvic pain, sometimes mimicking gynaecological conditions
- Chronic venous insufficiency — skin changes, varicosities, and venous ulcers in longstanding cases
Diagnosis
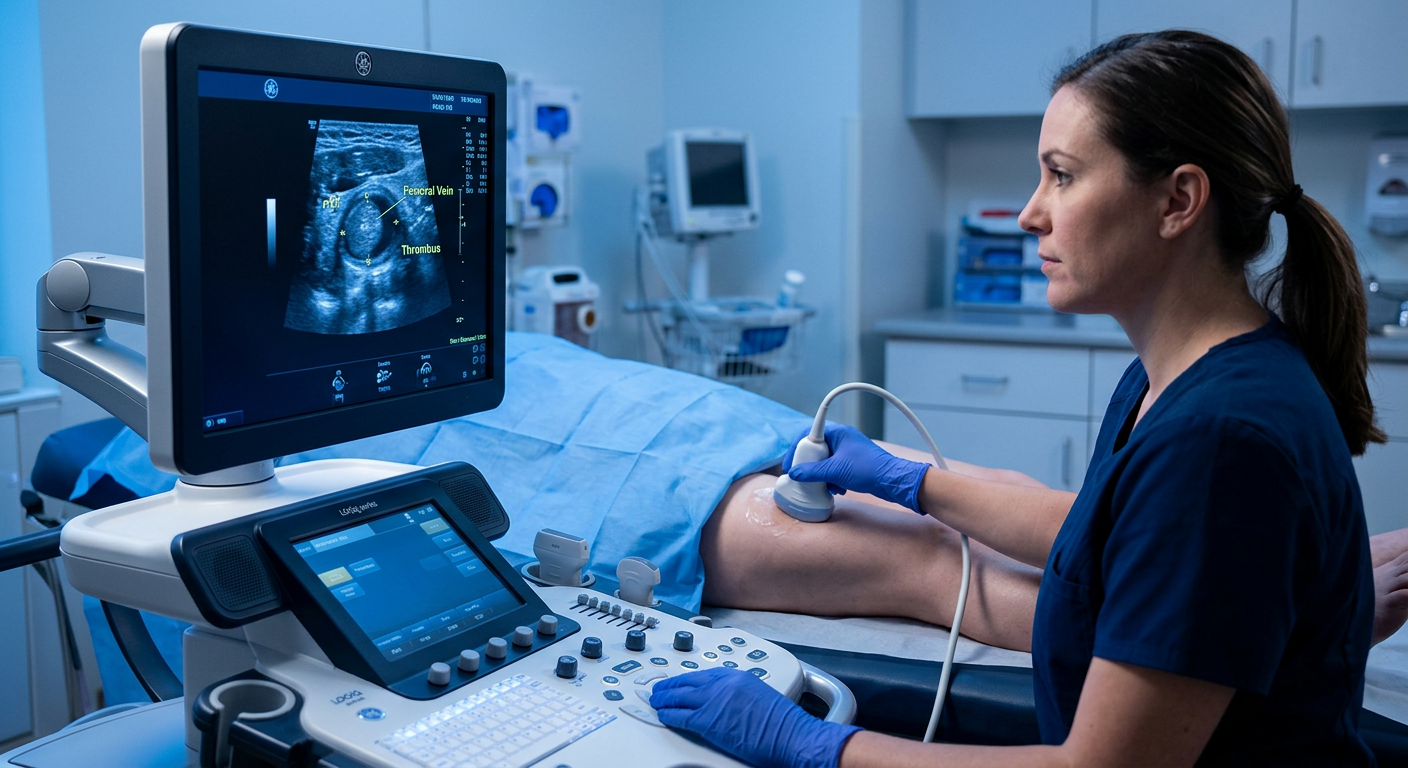
Because the compression occurs deep in the pelvis, standard leg duplex ultrasound will detect the DVT but not its underlying cause. Dedicated investigations include:
- CT venography (CTV): The most practical and widely available test — intravenous contrast outlines the iliac veins and clearly shows compression, collateral formation, and any filling defect from thrombus.
- MR venography (MRV): Excellent anatomical detail without radiation — preferred in younger patients where radiation minimisation is important.
- Intravascular ultrasound (IVUS): Performed at the time of catheter-based intervention — the gold standard for quantifying the degree of compression before stent deployment.
- Conventional venography: Historically the standard, now largely replaced by CTV and MRV for diagnosis; still used as part of the interventional procedure.
Treatment: Venous Stenting
The definitive treatment for symptomatic May-Thurner syndrome is endovascular — a catheter-based procedure performed by Dr. Haggag that typically involves three steps:
- Catheter-directed thrombolysis (CDT): If an acute DVT is present, a catheter is threaded into the clotted vein and a thrombolytic drug (tPA) is infused over 12–48 hours to dissolve the clot and restore venous patency.
- Balloon venoplasty: Once the vein is open, a balloon catheter dilates the compressed segment.
- Venous stent placement: A self-expanding dedicated venous stent is deployed across the compression point to hold the vein open permanently, abolishing the anatomical bottleneck.
The procedure is performed under local anaesthesia via a small groin puncture. Most patients go home the next day on anticoagulation, which is typically continued for 3–6 months to protect the stent while it endothelialises.
Outcomes
Results of venous stenting for May-Thurner are excellent:
- Primary patency (stent remains open without re-intervention) at 1 year: approximately 85–90%
- Assisted primary patency at 2 years: >95% with appropriate anticoagulation follow-up
- Significant improvement in leg swelling, pain, and quality of life reported by the majority of patients
- Prevention of further DVT episodes in most patients
Prevention of Recurrence
After stenting, patients should:
- Complete the prescribed anticoagulation course and attend regular follow-up
- Avoid combined oral contraceptives — discuss alternative contraception with their gynaecologist
- Wear graduated compression stockings as directed
- Stay active and well hydrated, particularly on long flights or car journeys
Left Leg Swelling with No Obvious Cause?
If you have unexplained left leg DVT or chronic left leg swelling — especially without obvious risk factors — May-Thurner syndrome may be the answer. Dr. Mohamed Haggag can arrange the appropriate imaging and, if confirmed, treat it with minimally invasive venous stenting.
Book a Consultation