Leg varicose veins are not just a cosmetic concern, and they are not a single disease with a single treatment. They are part of a spectrum called chronic venous disease that ranges from thin spider veins visible just below the skin, through classic tortuous bulging veins, all the way to chronic non-healing venous ulcers that disable everyday life. In this comprehensive guide, Dr. Mohamed Haggag — consultant vascular surgeon in Heliopolis, Cairo — walks through every layer of leg varicose veins: what they are, why they happen, the internationally recognized CEAP grading system that tells you where your case sits, how they are diagnosed, and the full modern treatment toolkit available today, from sclerotherapy to thermal ablation, glue closure, and surgical options.
What Are Leg Varicose Veins?
Varicose veins are enlarged, twisted superficial veins resulting from failure of the venous valves. In a healthy leg, the one-way valves inside veins — along with the calf muscle pump — propel blood back up to the heart against gravity. When those valves become incompetent, blood pools in the superficial system, vein walls stretch, and the characteristic bulging pattern emerges under the skin.
Varicose veins are far more common than most people realize: around 25–33% of women and 10–20% of men develop them at some point in life. Vascular surgery is the specialty best equipped to evaluate and treat them because it brings together accurate venous duplex diagnostics and the complete treatment toolkit — from injections and thermal catheters to open surgery — under one specialty.
Causes and Risk Factors
- Genetics: With one affected parent, risk is ~40%; with two affected parents, over 85%. Deep dive: Hereditary Varicose Veins.
- Pregnancy: Hormonal shifts, increased blood volume, and pelvic pressure either reveal or worsen varicose veins. See Varicose Veins During Pregnancy.
- Age: Valve competence declines with years of gravitational load.
- Female sex: Women are affected about 3× more often than men.
- Prolonged standing occupations: teachers, nurses, factory workers, hairdressers.
- Obesity: extra venous pressure below the waist.
- Sedentary lifestyle: the calf muscle pump stays idle.
- Onset in young adults: varicose veins are not confined to older patients — see Varicose Veins in Young Adults.
- Previous DVT: damages valves and causes secondary varicosities.
Symptoms and Warning Signs
- Visible bulging, twisted blue or greenish veins under the skin
- Leg heaviness and fatigue worse at the end of the day
- Burning, throbbing or tingling sensations
- Ankle swelling in the evening
- Nocturnal leg cramps
- Itching over the affected veins
- Brown hemosiderin staining around the ankle
- Dry, scaly "venous eczema" as disease progresses
- Chronic non-healing venous ulcers — the most serious complication
- Severe redness and pain along a vein (superficial phlebitis)
- Bleeding from a varicose vein
- A breakdown or ulcer at the ankle or lower leg
- Sudden discoloration of the leg
- Sudden swelling of one leg only (suspected deep vein thrombosis)
The CEAP Classification
Vascular surgeons worldwide use the CEAP system (Clinical–Etiologic–Anatomic–Pathophysiologic) to grade chronic venous disease. Day-to-day, the clinical axis (C) is what guides your management plan:
- C0: No visible or palpable signs of venous disease
- C1: Spider veins / telangiectasias under 3 mm
- C2: True varicose veins larger than 3 mm
- C3: Varicose veins with leg edema
- C4: Skin changes (pigmentation, venous eczema, lipodermatosclerosis)
- C5: Healed venous ulcer
- C6: Active venous ulcer
This grading drives the strategy: C1–C2 can often be treated in the clinic without any surgery, while C4–C6 usually need a more comprehensive, staged approach and long-term follow-up.
How Varicose Veins Are Diagnosed
- Focused clinical examination: Standing inspection, palpation along the saphenous axes, reflux tests.
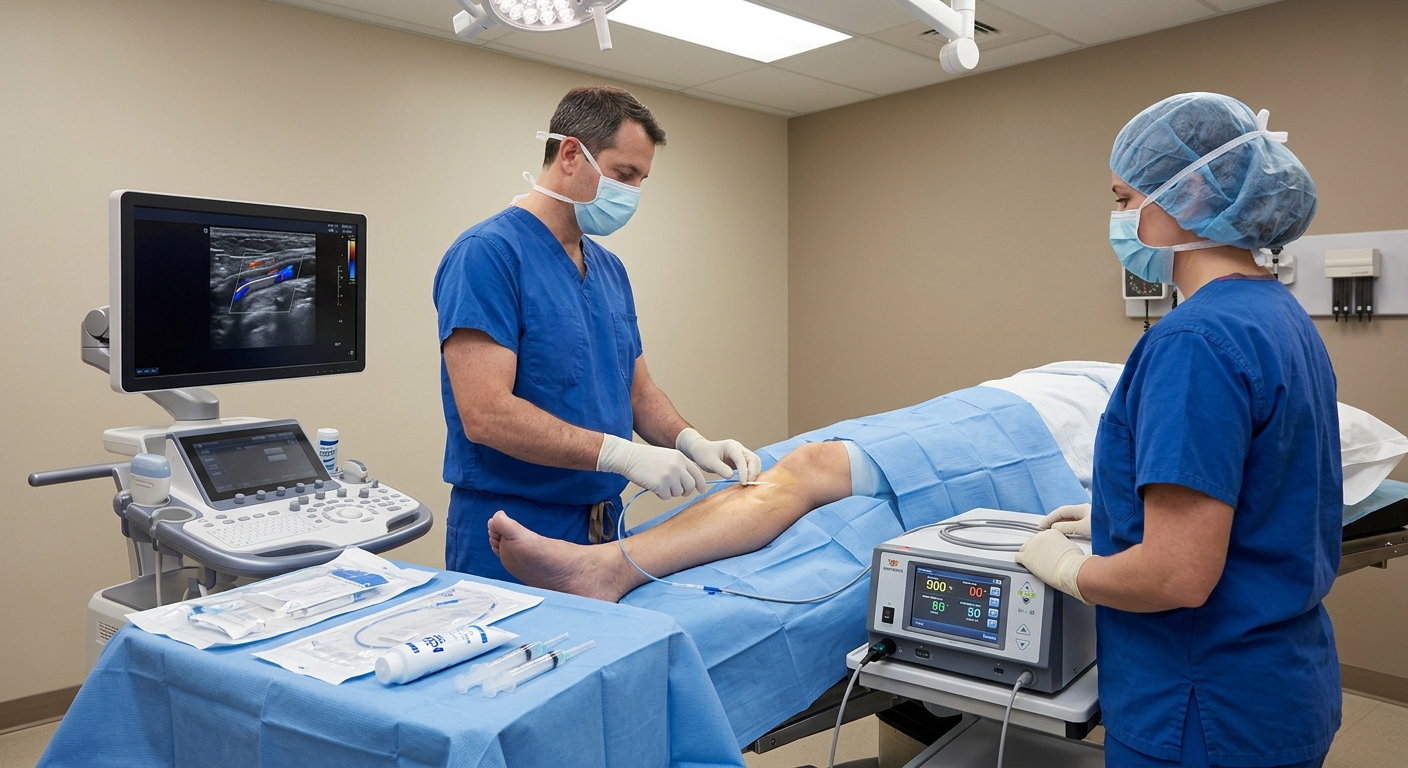
- Venous duplex ultrasound: The gold standard — confirms reflux, quantifies its duration, and maps the incompetent veins precisely.
- Venous pressure studies: Reserved for complex or recurrent cases.
- CT or MR venography: When deep venous obstruction is suspected (e.g., May–Thurner syndrome).
- Contrast venography: Rarely diagnostic now — used during interventional procedures.
The Modern Treatment Toolkit
The right treatment depends on the CEAP grade, which vein is incompetent (great saphenous, small saphenous, or tributaries), symptoms, and patient factors. The modern options are:
- Conservative care & lifestyle: Graduated compression stockings, weight reduction, leg elevation, walking.
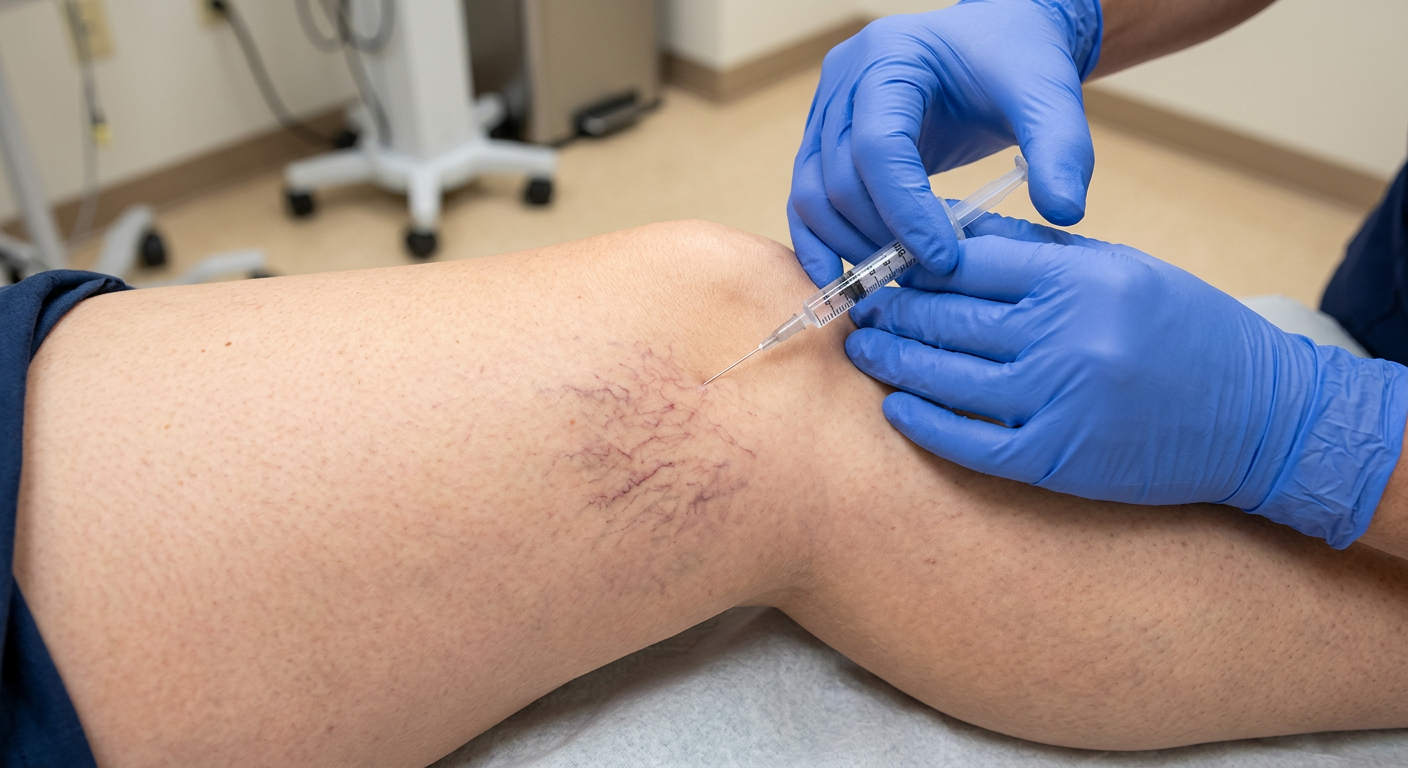
- Sclerotherapy: Injection of a sclerosant into small and spider veins — ideal for C1 disease. See Cosmetic Vein Treatment.
- Endovenous Laser Ablation (EVLA): A laser catheter inserted into the faulty vein closes it from inside — a minimally invasive replacement for stripping. See Thermal Laser Treatment.
- Radiofrequency Ablation (RFA): Same principle using radiofrequency energy — excellent outcomes and typically less post-procedure pain. Read Radiofrequency Ablation for Varicose Veins.
- MOCA (Mechanochemical Ablation): Combines mechanical and chemical injury — a non-thermal option.
- VenaSeal (medical adhesive): A cyanoacrylate glue that seals the vein immediately, without heat or tumescent anesthesia.
- Open surgery (stripping): Now reserved for selected cases — compare the choice in Laser vs Traditional Surgery.
- Ambulatory phlebectomy: Removal of bulging tributary varices through tiny skin punctures.
In most cases these modalities are combined in a single session — for example, EVLA of the great saphenous trunk + phlebectomy of prominent tributaries + later sclerotherapy for residual spider veins — to achieve the best overall cosmetic and functional result.
Prevention and Lifestyle
- Walk at least 30 minutes daily — engage the calf muscle pump
- Avoid prolonged motionless standing or sitting
- Elevate your legs for 10–15 minutes several times a day
- Wear graduated compression stockings on long flights and in standing occupations
- Maintain a healthy weight
- Avoid very tight clothing and high heels for long periods
- Stay hydrated and eat a fiber-rich diet to prevent constipation
Suffering From Varicose Veins? Book a Complete Assessment
Get a full venous duplex evaluation and a tailored treatment plan at Dr. Mohamed Haggag's clinic in Heliopolis, Cairo. Every modern varicose vein technique — under one roof, with 11 years of dedicated vascular surgery experience.
Book a Consultation